 https://doi.org/10.4081/ejtm.2026.15083
https://doi.org/10.4081/ejtm.2026.15083
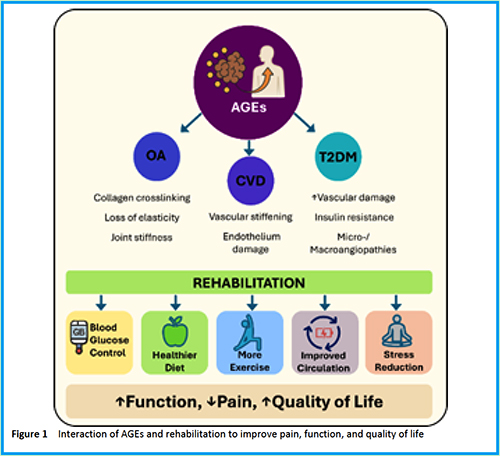
Abstract 084 | Explorative evidence on the sensitivity and specificity of advanced glycation endproducts in reflecting functional recovery during multimodal rehabilitation
Bettina Thauerer, Bibiane Steinecker-Frohnwieser | Ludwig Boltzmann Institute for Arthritis and Rehabilitation, Saalfelden, Gröbming, Vienna, Austria.
All claims expressed in this article are solely those of the authors and do not necessarily represent those of their affiliated organizations, or those of the publisher, the editors and the reviewers. Any product that may be evaluated in this article or claim that may be made by its manufacturer is not guaranteed or endorsed by the publisher.
Published: 2 March 2026
Downloads
1. Hooshiar SH, Esmaili H, Taherian A, & Jafarnejad S. Exercise, Advanced Glycation End Products, and Their Effects on Cardiovascular Disorders: A Narrative Review. Heart and Mind 6(3), 2022. DOI: 10.4103/hm.hm_31_22.
2. Lin H, Yang Y, Wang X, Chung M, Zhang L, Cai S, Pan X, Pan Y. Targeting the AGEs-RAGE axis: pathogenic mechanisms and therapeutic interventions in diabetic wound healing. Front. Med., Sec. Translational Medicine 12, 2025. DOI:10.3389/fmed.2025.1667620.
3. He CP, Chen C, Jiang XC, Li H, Zhu LX, Wang PX, Xiao T. The role of AGEs in pathogenesis of cartilage destruction in osteoarthritis. Bone Joint Res., 11(5), 2022. DOI:10.1302/2046-3758.
4. Odrovicsné-Tóth A, Thauerer B, Stritzinger B, Kullich W, Salzer A, Skoumal M, Steinecker-Frohnwieser B. The Patient’s Physiological Status at the Start Determines the Success of the Inpatient Cardiovascular Rehabilitation Program. J. Clin. Med.12, 2023. DOI:10.3390/jcm12051735.
5. Zhang Y, Zhang Z, Tu C, Chen X, He R. Advanced Glycation End Products in Disease Development and Potential Interventions. Antioxidants 14, 2025. DOI:10.3390/antiox14040492.
6. Thauerer B, Odrovicsné Tóth A, Salzer A, Steinecker-Frohnwieser B. Success of an Inpatient Rehabilitation Program in Subjects with Type 2 Diabetes Mellitus with or Without Metabolic Syndrome. Biomolecules 14, 2024. DOI:10.3390/biom14121527.
7. Thauerer, B, Odrovicsné Tóth A, Salzer A, Steinecker-Frohnwieser B. Osteoarthritis and Cartilage 32, 2024. DOI:10.1016/j.joca.2024.02.195.
How to Cite

This work is licensed under a Creative Commons Attribution-NonCommercial 4.0 International License.
PAGEPress has chosen to apply the Creative Commons Attribution NonCommercial 4.0 International License (CC BY-NC 4.0) to all manuscripts to be published.

