 https://doi.org/10.4081/ejtm.2021.9411
https://doi.org/10.4081/ejtm.2021.9411
Burnout among Iranian medical students: Prevalence and its relationship to personality dimensions and physical activity
All claims expressed in this article are solely those of the authors and do not necessarily represent those of their affiliated organizations, or those of the publisher, the editors and the reviewers. Any product that may be evaluated in this article or claim that may be made by its manufacturer is not guaranteed or endorsed by the publisher.
Published: 5 February 2021
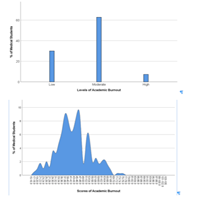
Several studies have shown the association between personality traits and academic burnout. But the main goal of the present study was to find out an experimental answer to the following questions: Is there a simple relationship between personality dimensions and academic burnout? Can physical activity affect this relationship?. In this cross-sectional correlational study, 417 medical students were selected from three major cities of Iran through stratified multistage sampling and assessed by demographic information form, Baecke Physical Activity Questionnaire, Temperament and Character Inventory, and Breso’s Academic Burnout Questionnaire. Bivariate Pearson correlations and hierarchical linear regression were used to examine the relationships between academic burnout, personality traits, and physical activity. In this study, 400 medical students (39% male and 61% female) filled the questionnaires correctly. The total prevalence of academic burnout was 25.5% (n=102), with heterogeneous levels. Regression analysis indicated that in a multivariate model, being male (β=0.08, p=0.013), higher years of medical school (β=0.18, p˂0.001), and lower scores in novelty seeking (β=-0.53, p=0.006), cooperativeness (β=-0.55, p=0.010), and physical activity (β=-1.22, p˂0.001) could be attributed to higher scores of academic burnout. Furthermore, physical activity had a moderating role in “novelty seeking-academic burnout” (β=-0.47, p=0.044) and “cooperativeness-academic burnout” (β=-0.89, p=0.001) relationships (ΔR2=0.02, p˂0.001). The results suggested that male gender, higher years of medical school, and lower levels of novelty seeking, cooperativeness, and physical activity are associated with higher levels of academic burnout among Iranian medical students. Therefore, paying attention to male gender and individual difference factors, as well as planning for physical education classes during the medicine courses (especially in the last years of medical school), seems essential. However, more extensive investigations need to be carried out in this field through longitudinal studies.
Downloads
Charkhabi M, Abarghuei MA, Hayati D. The association of academic burnout with self-efficacy and quality of learning experience among Iranian students. Springerplus. 2013;2(1):677. DOI: https://doi.org/10.1186/2193-1801-2-677
Schaufeli WB, Martinez IM, Pinto AM, Salanova M, Bakker AB. Burnout and engagement in university students: A cross-national study. J Cross Cult Psychol. 2002;33(5):464-81. DOI: https://doi.org/10.1177/0022022102033005003
Kafry D, Pines A. The experience of tedium in life and work. Human Relations. 1980;33(7):477-503. DOI: https://doi.org/10.1177/001872678003300703
Dyrbye L, Shanafelt T. A narrative review on burnout experienced by medical students and residents. Med Educ. 2016;50(1):132-49. DOI: https://doi.org/10.1111/medu.12927
Maslach C, Jackson SE. The measurement of experienced burnout. J Organ Behav. 1981;2(2):99- 113. DOI: https://doi.org/10.1002/job.4030020205
Romani M, Ashkar K. Burnout among physicians. Libyan J Med. 2014;9(1):23556. DOI: https://doi.org/10.3402/ljm.v9.23556
Lee SJ, Choi YJ, Chae H. The effects of personality traits on academic burnout in Korean medical students. Integr Med Res. 2017;6(2):207-13. doi: 10.1016/j.imr.2017.03.005. DOI: https://doi.org/10.1016/j.imr.2017.03.005
Lyndon MP, Henning MA, Alyami H, Krishna S, Zeng I, Yu TC, Hill AG. Burnout, quality of life, motivation, and academic achievement among medical students: A person-oriented approach. Perspect Med Educ. 2017;6(2):108-14. DOI: https://doi.org/10.1007/s40037-017-0340-6
ElKholy MM, El-Sayed ET, Sedrak AS, Raouf NA. Prevalence and Predictors of Burnout Syndrome among Medical Students of Cairo University. Egyptian Journal of Community Medicine. 2019;37(3):83-93. DOI: https://doi.org/10.21608/ejcm.2019.43375
Kumar S. Burnout and doctors: prevalence, prevention and intervention. Healthcare. 2016;4(3):37. DOI: https://doi.org/10.3390/healthcare4030037
Dyrbye LN, Thomas MR, Massie FS, Power DV, Eacker A, Harper W, Durning S, Moutier C, Szydlo DW, Novotny PJ, Sloan JA, Shanafelt TD. Burnout and suicidal ideation among US medical students. Ann Intern Med. 2008;149(5):334-41. DOI: https://doi.org/10.7326/0003-4819-149-5-200809020-00008
Erschens R, Keifenheim KE, Herrmann-Werner A, Loda T, Schwille-Kiuntke J, Bugaj TJ, Nikendei C, Huhn D, Zipfel S, Junne F. Professional burnout among medical students: Systematic literature review and meta-analysis. Med Teach. 2019;41(2):172-83. DOI: https://doi.org/10.1080/0142159X.2018.1457213
LianP,SunY,JiZ,LiH,PengJ.Movingawayfrom exhaustion: how core self-evaluations influence academic burnout. PLoS One. 2014;9(1):e87152. DOI: https://doi.org/10.1371/journal.pone.0087152
Zhang Y, Gan Y, Cham H. Perfectionism, academic burnout and engagement among Chinese college students: A structural equation modeling analysis. Pers Individ Dif. 2007;43(6):1529-40. DOI: https://doi.org/10.1016/j.paid.2007.04.010
Yang HJ, Farn CK. An investigation the factors affecting MIS student burnout in technical- vocational college. Comput Human Behav. 2005;21(6):917-32. DOI: https://doi.org/10.1016/j.chb.2004.03.001
Slivar B. The syndrome of burnout, self-image, and anxiety with grammar school students. Horizons of Psychology. 2001;10(2):21-32.
JacobsSR,DoddD.Studentburnoutasafunctionof personality, social support, and workload. J Coll Stud Dev. 2003;44(3):291-303. DOI: https://doi.org/10.1353/csd.2003.0028
Jiang N, Sato T, Hara T, Takedomi Y, Ozaki I, Yamada S. Correlations between trait anxiety, personality and fatigue: study based on the Temperament and Character Inventory. J Psychosom Res. 2003;55(6):493-500. DOI: https://doi.org/10.1016/S0022-3999(03)00021-7
Raycheva RD, Asenova RS, Kazakov DN, Yordanov SY, Tarnovska T, Stoyanov DS. The vulnerability to burn out in healthcare personnel according to the Stoyanov-Cloninger model: evidence from a pilot study. Int J Pers Cent Med. 2012;2(3):552-63.
Melchers MC, Plieger T, Meermann R, Reuter M. Differentiating burnout from depression: personality matters! Front Psychiatry. 2015;6:113. DOI: https://doi.org/10.3389/fpsyt.2015.00113
Yazici AB, Esen O, Yazici E, Esen H, Ince M. The relationship between temperament and character traits and burnout among nurses. Journal of Psychology & Psychotherapy. 2014;4(5):1-5.
Stoyanov DS, Cloninger CR. Relation of people- centered public health and person-centered healthcare management: a case study to reduce burnout. Int J Pers Cent Med. 2012;2(1):90-5.
Macilwrait P, Bennett D. Burnout and physical activity in medical students. Ir Med J. 2018;111(3):707.
Khosravi M, Mirbahaadin M, Kasaeiyan R. Understanding the influence of high novelty-seeking on academic burnout: Moderating effect of physical activity. Eur J Transl Myol. 2020;30(2):318-24. DOI: https://doi.org/10.4081/ejtm.2020.8722
Weight CJ, Sellon JL, Lessard-Anderson CR, Shanafelt TD, Olsen KD, Laskowski ER. Physical activity, quality of life, and burnout among physician trainees: the effect of a team-based, incentivized exercise program. Mayo Clin Proc. 2013;88(12):1435-42. DOI: https://doi.org/10.1016/j.mayocp.2013.09.010
Gerber M, Brand S, Elliot C, Holsboer-Trachsler E, Pühse U, Beck J. Aerobic exercise training and burnout: a pilot study with male participants suffering from burnout. BMC Res Notes. 2013;6:78. DOI: https://doi.org/10.1186/1756-0500-6-78
Sadeghisani M, Manshadi FD, Azimi H, Montazeri A. Validity and reliability of the Persian version of Baecke habitual physical activity questionnaire in healthy subjects. Asian journal of sports medicine. Asian J Sports Med. 2016;7(3):e31778. DOI: https://doi.org/10.5812/asjsm.31778
Dadfar M, Bahrami F, Dadfar F, Younesi SJ. Reliability and validity of the Temperament and Character Inventory. Journal of Rehabilitation. 2010;11(3):15-24. (Persian)
Marzoghi R, Haidari M, Haidari A. The impact of educational justice on students’ academic burnout in the University of Social Welfare and Rehabilitation Science, Tehran, Iran. Strides in Development of Medical Education Journal. 2012;10(3):328–34. (Persian)
Dyrbye LN, West CP, Satele D, Boone S, Tan L, Sloan J, Shanafelt TD. Burnout among US medical students, residents, and early career physicians relative to the general US population. Acad Med. 2014;89(3):443-51. doi: 10.1097/ACM.000000000 0000134.
Chin RW, Chua YY, Chu MN, Yusoff MSB, Wong MS, Lee YY Prevalence of Burnout among Universiti Sains Malaysia Medical Students. Education in Medicine Journal. 2016;8(3):61-74. DOI: https://doi.org/10.5959/eimj.v8i3.454
Dunn LB, Iglewicz A, Moutier C. A conceptual model of medical student well-being: promoting resilience and preventing burnout. Acad Psychiatry. 2008;32(1):44-53. DOI: https://doi.org/10.1176/appi.ap.32.1.44
Dyrbye LN, Thomas MR, Huntington JL, Lawson KL, Novotny PJ, Sloan JA, Shanafelt TD.Personal life events and medical student burnout: a multicenter study. Acad Med. 2006;81(4):374-84. DOI: https://doi.org/10.1097/00001888-200604000-00010
Santen SA, Holt DB, Kemp JD, Hemphill RR. Burnout in medical students: examining the prevalence and associated factors. South Med J. 2010;103(8):758-63. DOI: https://doi.org/10.1097/SMJ.0b013e3181e6d6d4
Willcock SM, Daly MG, Tennant CC, Allard BJ. Burnout and psychiatric morbidity in new medical graduates. Med J Aust. 2004;181(7):357-60. DOI: https://doi.org/10.5694/j.1326-5377.2004.tb06325.x
Lee KP, Yeung N, Wong C, Yip B, Luk LH, Wong S. Prevalence of medical students’ burnout and its associated demographics and lifestyle factors in Hong Kong. PLoS One. 2020;15(7):e0235154. DOI: https://doi.org/10.1371/journal.pone.0235154
Webb E, Ashton CH, Kelly P, Kamali F. An update on British medical students’ lifestyles. Med Educ. 1998;32(3):325-31. DOI: https://doi.org/10.1046/j.1365-2923.1998.00204.x
Hao W, Yi H, Liu Z, GaoY, Eshita Y, Guo W, Zhang H, Sun J. Gender comparisons of physical fitness indexes in Inner Mongolia medical students in China. Glob J Health Sci. 2014;7(1):220-7. DOI: https://doi.org/10.5539/gjhs.v7n1p220
Ball S, Bax A. Self-care in medical education: effectiveness of health-habits interventions for first- year medical students. Acad Med. 2002;77(9):911- 7. DOI: https://doi.org/10.1097/00001888-200209000-00023
Frank E, Carrera JS, Elon L, Hertzberg VS. Basic demographics, health practices, and health status of US medical students. Am J Prev Med. 2006;31(6):499-505. DOI: https://doi.org/10.1016/j.amepre.2006.08.009
Peterson DF, Degenhardt BF, Smith CM. Correlation between prior exercise and present health and fitness status of entering medical students. J Am Osteopath Assoc. 2003;103(8):361-6.
Boni RA, Paiva CE, De Oliveira MA, Lucchetti G, Fregnani JH, Paiva BS. Burnout among medical students during the first years of undergraduate school: Prevalence and associated factors. PLoS One. 2018;13(3):e0191746. DOI: https://doi.org/10.1371/journal.pone.0191746
Cecil J, McHale C, Hart J, Laidlaw A. Behavior and burnout in medical students. Med Educ Online. 2014;19(1):25209. DOI: https://doi.org/10.3402/meo.v19.25209
Barlow DH, Allen LB, Choate ML. Toward a unified treatment for emotional disorders–republished article. Behav Ther. 2016;47(6):838-53. DOI: https://doi.org/10.1016/j.beth.2016.11.005
Likus W, Milka D, Bajor G, Jachacz-Lopata M, Dorzak B. Dietary habits and physical activity in students from the Medical University of Silesia in Poland. Rocz Panstw Zakl Hig. 2013;64(4):317-24.
Armon G. Type D personality and job burnout: The moderating role of physical activity. Pers Individ Dif. 2014;58:112-5. DOI: https://doi.org/10.1016/j.paid.2013.10.020
Lumley S, Ward P, Roberts L, Mann JP. Self- reported extracurricular activity, academic success, and quality of life in UK medical students. Int J Med Educ. 2015;6:111-7. DOI: https://doi.org/10.5116/ijme.55f8.5f04
How to Cite
PAGEPress has chosen to apply the Creative Commons Attribution NonCommercial 4.0 International License (CC BY-NC 4.0) to all manuscripts to be published.

